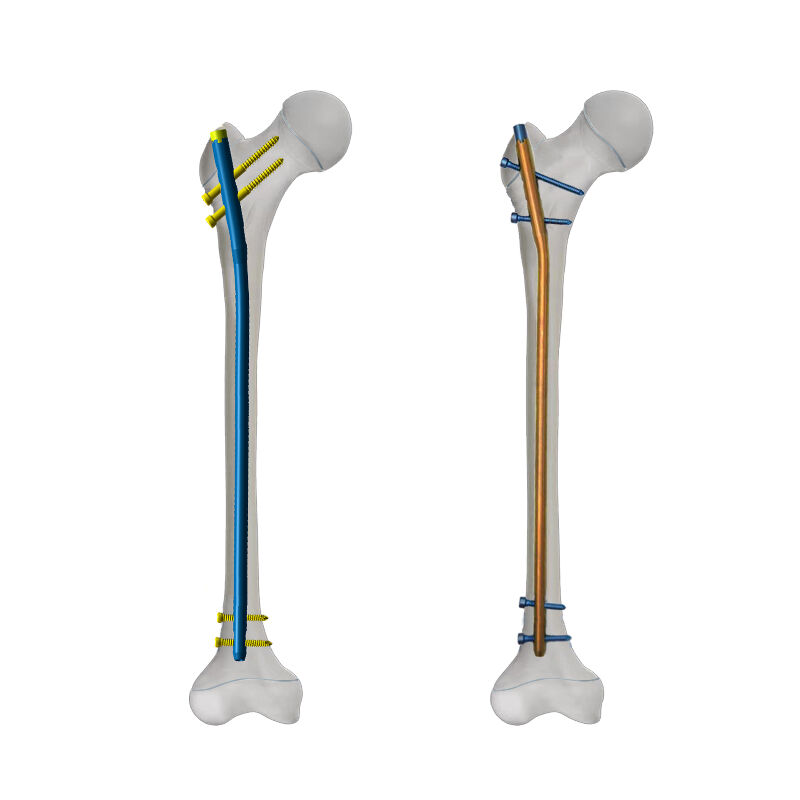
Modern orthopedic surgery continues to evolve with innovative solutions that address complex fracture patterns and deformity corrections. The telescopic intramedullary nail represents a significant advancement in treating challenging periarticular fractures and managing limb length discrepancies. This revolutionary implant technology extends beyond traditional intramedullary nailing techniques, offering surgeons enhanced versatility in treating patients with complex skeletal injuries and congenital deformities
The clinical applications of telescopic intramedullary nail systems have expanded dramatically over recent years, particularly in addressing periarticular fractures that were previously considered unsuitable for standard intramedullary fixation. These implants provide controlled lengthening capabilities while maintaining mechanical stability throughout the healing process. The integration of telescopic mechanisms within the nail design allows for gradual distraction and compression forces, essential for managing complex deformity corrections and fracture healing optimization.

Advanced Applications in Periarticular Fracture Management
Proximal Femoral Fracture Treatment
Proximal femoral fractures present unique challenges in orthopedic surgery, particularly when dealing with comminuted patterns near the greater trochanter region. The telescopic intramedullary nail system offers superior mechanical advantages compared to conventional implants in these scenarios. The adjustable length feature allows surgeons to accommodate varying bone geometry while maintaining optimal mechanical alignment throughout the healing process.
Clinical studies demonstrate that telescopic intramedullary nail applications in proximal femoral fractures result in improved functional outcomes and reduced complications. The ability to fine-tune the implant length post-operatively provides surgeons with unprecedented control over fracture reduction and maintenance. This technology particularly benefits patients with osteoporotic bone quality, where traditional fixation methods may fail due to inadequate purchase in compromised bone stock.
Distal Tibial and Periarticular Injuries
Distal tibial fractures extending into the metaphyseal region have historically posed significant treatment challenges. The telescopic intramedullary nail technology addresses these challenges by providing stable fixation while allowing for controlled compression or distraction as needed. The expandable design accommodates the varying canal diameter from diaphyseal to metaphyseal regions, ensuring optimal fit and stability.
The versatility of telescopic intramedullary nail systems enables surgeons to manage complex periarticular injuries with greater precision. These implants can be adjusted to compensate for bone loss, accommodate varying patient anatomy, and provide sustained mechanical support throughout the healing process. The technology has proven particularly valuable in revision surgeries where bone stock may be compromised or altered from previous interventions.
Deformity Correction Capabilities
Limb Length Discrepancy Management
Limb length discrepancies resulting from trauma, infection, or congenital conditions require precise correction strategies. The telescopic intramedullary nail provides controlled lengthening capabilities that can be adjusted gradually over time. This approach minimizes the risk of neurovascular complications while achieving optimal limb length restoration.
The internal lengthening mechanism of telescopic intramedullary nail systems eliminates the need for external fixation devices in many cases. Patients benefit from improved comfort, reduced infection risk, and enhanced quality of life during the correction process. The precise control over lengthening rates allows for optimal tissue adaptation and bone formation, resulting in superior clinical outcomes compared to traditional external fixation methods.

Angular Deformity Correction
Angular deformities in long bones require careful planning and execution to achieve optimal alignment. Telescopic intramedullary nail technology can be combined with osteotomy procedures to address both angular and length corrections simultaneously. The adjustable nature of these implants allows for fine-tuning of corrections throughout the healing process, ensuring optimal final alignment.
The biomechanical properties of telescopic intramedullary nail systems provide excellent support during the deformity correction process. The internal structure maintains mechanical stability while allowing for controlled movement, essential for achieving gradual correction without compromising bone healing. This technology has revolutionized the treatment of complex deformities that previously required multiple surgical procedures or external fixation methods.
Technical Considerations and Surgical Techniques
Preoperative Planning and Assessment
Successful implementation of telescopic intramedullary nail technology requires comprehensive preoperative planning. Advanced imaging techniques, including CT scans and three-dimensional reconstructions, help surgeons determine optimal implant sizing and positioning. The expandable nature of these implants requires careful consideration of canal dimensions and bone quality assessment.
Patient selection criteria for telescopic intramedullary nail procedures include bone quality assessment, fracture pattern analysis, and overall medical condition evaluation. The versatility of these implants allows for treatment of a broader range of patients compared to conventional intramedullary nails. However, specific anatomical considerations must be addressed to ensure optimal outcomes and minimize complications.
Surgical Technique Modifications
The surgical technique for telescopic intramedullary nail insertion requires modifications compared to standard intramedullary nailing procedures. The expandable mechanism necessitates careful attention to proper positioning and activation protocols. Surgeons must be familiar with the specific activation mechanisms and adjustment procedures unique to each telescopic intramedullary nail system.
Postoperative management protocols for telescopic intramedullary nail patients differ from standard intramedullary nailing procedures. The ability to make adjustments during the healing process requires regular monitoring and assessment. Imaging studies help track bone healing progress and determine optimal timing for length or compression adjustments throughout the treatment course.
Clinical Outcomes and Patient Benefits
Functional Recovery Advantages
Patients treated with telescopic intramedullary nail systems demonstrate superior functional recovery compared to traditional external fixation methods. The internal nature of the implant allows for earlier mobilization and weight-bearing activities. Studies show improved patient satisfaction scores and reduced complications associated with external pin sites and bulky external frames.
The precision of telescopic intramedullary nail adjustments results in more accurate final corrections and improved long-term outcomes. Patients benefit from reduced treatment duration and fewer surgical procedures compared to alternative treatment methods. The technology enables surgeons to achieve optimal results while minimizing patient discomfort and maximizing functional recovery potential.
Complication Reduction and Management
Telescopic intramedullary nail technology has demonstrated reduced complication rates compared to external fixation methods for similar indications. The internal fixation eliminates pin site infections and reduces the risk of neurovascular injury associated with external frames. The controlled adjustment mechanism minimizes the risk of over-distraction or under-correction commonly seen with other treatment methods.
Long-term follow-up studies of telescopic intramedullary nail patients show excellent implant survival rates and sustained functional improvements. The robust design of these implants provides durable fixation while accommodating the dynamic nature of bone healing and remodeling. Revision surgery rates are significantly lower compared to external fixation methods for similar clinical indications.
Future Developments and Innovations
Technological Advancements
Ongoing research and development in telescopic intramedullary nail technology focuses on improving adjustment mechanisms and expanding clinical applications. Smart implants with remote-controlled adjustment capabilities are under development, potentially eliminating the need for multiple surgical procedures during the correction process. These advances promise to further improve patient outcomes and surgical efficiency.
Biomaterial improvements in telescopic intramedullary nail design include enhanced corrosion resistance and improved biocompatibility. Surface treatments and coating technologies are being developed to promote better bone integration and reduce long-term complications. These innovations will likely expand the patient population suitable for telescopic intramedullary nail treatment.
Expanded Clinical Applications
The versatility of telescopic intramedullary nail systems continues to expand into new clinical applications. Research is ongoing into their use for pediatric deformity corrections, tumor reconstruction procedures, and complex revision surgeries. The adaptable nature of these implants makes them suitable for addressing previously challenging clinical scenarios.
Integration of telescopic intramedullary nail technology with computer-assisted surgery and robotic systems represents the next frontier in orthopedic innovation. These combinations promise to further improve precision and outcomes while reducing surgical complexity and operative time. The future of telescopic intramedullary nail applications appears promising with continued technological advancement and clinical research.
FAQ
What makes telescopic intramedullary nails different from standard intramedullary nails?
Telescopic intramedullary nails feature an internal mechanism that allows for length adjustment after implantation, unlike standard nails with fixed dimensions. This adjustability enables controlled lengthening or compression during the healing process, making them ideal for deformity correction and complex fracture management. The technology provides surgeons with unprecedented control over fracture healing and limb alignment restoration.
How long does the adjustment process take when using telescopic intramedullary nails?
The adjustment timeline varies depending on the specific clinical indication and desired correction amount. Typical lengthening procedures progress at rates of 0.5 to 1.0 millimeters per day, allowing tissues to adapt gradually. Complete corrections may take several months, but the internal nature of the telescopic intramedullary nail allows patients to maintain normal activities throughout the process, unlike external fixation methods.
Are there specific patient criteria for telescopic intramedullary nail treatment?
Patient selection for telescopic intramedullary nail procedures considers bone quality, fracture pattern complexity, and overall health status. These implants are particularly beneficial for patients with limb length discrepancies, complex periarticular fractures, or deformity corrections. Age is not necessarily a limiting factor, as these systems have been successfully used in both pediatric and adult populations with appropriate modifications.
What are the long-term outcomes for patients treated with telescopic intramedullary nails?
Long-term studies demonstrate excellent functional outcomes and high patient satisfaction rates with telescopic intramedullary nail treatment. Most patients achieve their target corrections with minimal complications and return to normal activities. The implants show excellent durability and biocompatibility, with low revision rates compared to alternative treatment methods for similar clinical conditions.
Table of Contents
- Advanced Applications in Periarticular Fracture Management
- Deformity Correction Capabilities
- Technical Considerations and Surgical Techniques
- Clinical Outcomes and Patient Benefits
- Future Developments and Innovations
-
FAQ
- What makes telescopic intramedullary nails different from standard intramedullary nails?
- How long does the adjustment process take when using telescopic intramedullary nails?
- Are there specific patient criteria for telescopic intramedullary nail treatment?
- What are the long-term outcomes for patients treated with telescopic intramedullary nails?