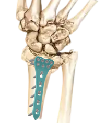
The treatment of distal radius fractures has undergone significant evolution in recent decades, with the distal radial volar locking plate emerging as a cornerstone technology in modern orthopedic practice. These innovative implants represent a paradigm shift from traditional fixation methods, offering surgeons enhanced control, improved stability, and superior patient outcomes. The refined design features of contemporary distal radial volar locking plates have revolutionized fracture fixation protocols, enabling more precise anatomical reconstruction and faster patient recovery times. Advanced manufacturing techniques and biomechanical engineering principles have culminated in implant designs that address the unique challenges posed by complex distal radius fractures.
Biomechanical Advantages of Modern Locking Plate Technology
Enhanced Stability Through Fixed-Angle Constructs
The fundamental biomechanical advantage of the distal radial volar locking plate lies in its fixed-angle construct, which provides superior stability compared to conventional plating systems. Unlike traditional plates that rely solely on friction between the plate and bone, locking plates create a rigid construct where screws lock into the plate at predetermined angles. This mechanism eliminates the risk of screw toggle and maintains reduction even in osteoporotic bone, a common challenge in elderly patients with distal radius fractures. The locked construct effectively transforms the plate-screw interface into a single beam, distributing loads more evenly across the fracture site and reducing stress concentrations that could lead to implant failure.
Clinical studies have demonstrated that the fixed-angle design significantly reduces the incidence of secondary displacement, particularly in unstable fracture patterns. The locking mechanism allows surgeons to maintain anatomical reduction without relying on bone quality for screw purchase, making the distal radial volar locking plate particularly valuable in treating fragility fractures. Advanced metallurgy and precision manufacturing ensure that the locking interface maintains its integrity throughout the healing process, providing consistent stability that promotes optimal fracture union.
![77472105 胫骨近端内侧加压锁定板 大型 5孔右 [5.0].png](https://shopcdnpro.grainajz.com/category/83036/2966/c0d52fb2c69f33244f15e433bdc702eb/77472105%20%E8%83%AB%E9%AA%A8%E8%BF%91%E7%AB%AF%E5%86%85%E4%BE%A7%E5%8A%A0%E5%8E%8B%E9%94%81%E5%AE%9A%E6%9D%BF%20%E5%A4%A7%E5%9E%8B%205%E5%AD%94%E5%8F%B3%20%5B5.0%5D.png)
Optimized Load Distribution Patterns
The sophisticated engineering behind modern distal radial volar locking plates incorporates finite element analysis to optimize load distribution patterns across the implant-bone interface. Strategic placement of locking holes and variable screw trajectories allow surgeons to customize the fixation construct based on individual fracture patterns and bone quality. This adaptability ensures that mechanical loads are distributed in a manner that promotes healing while minimizing stress shielding effects that could compromise long-term bone health.
Research has shown that properly designed locking plates can reduce peak stresses at the fracture site by up to 40% compared to conventional plating systems. The ability to place screws in multiple directions through a single hole provides additional fixation options in complex fractures, particularly those involving the articular surface. This versatility makes the distal radial volar locking plate an essential tool for addressing challenging fracture patterns that would be difficult to manage with traditional fixation methods.
Refined Design Features for Enhanced Surgical Outcomes
Anatomically Contoured Plate Geometry
Contemporary distal radial volar locking plates feature anatomically contoured geometries developed through extensive radiographic analysis of normal radius anatomy across diverse patient populations. These refined contours minimize the need for intraoperative plate bending, reducing surgical time and preserving implant strength. The pre-contoured design ensures optimal plate-to-bone contact, which is crucial for maintaining reduction and preventing soft tissue irritation that could lead to complications such as flexor tendon rupture.
Advanced imaging techniques and computer-aided design have enabled manufacturers to create plates that accommodate anatomical variations while maintaining consistent performance characteristics. The refined profile of modern distal radial volar locking plates features smooth edges and rounded corners that minimize interference with surrounding soft tissues. This attention to anatomical compatibility has significantly reduced the incidence of postoperative complications related to implant prominence and soft tissue irritation.
Variable Angle Locking Technology
The introduction of variable angle locking technology represents a significant advancement in distal radial volar locking plate design, providing surgeons with unprecedented flexibility in screw placement. This innovation allows screws to be inserted at angles up to 15 degrees from the perpendicular axis, enabling better capture of fracture fragments and avoidance of critical anatomical structures. The variable angle capability is particularly valuable when treating complex intra-articular fractures where precise subchondral bone support is essential for maintaining joint congruity.
Clinical applications of variable angle technology have demonstrated improved outcomes in challenging cases, including fractures with significant comminution or those occurring in patients with unusual anatomy. The ability to direct screws away from the watershed line or other critical areas reduces the risk of complications while maintaining strong fixation. This technological advancement has expanded the indications for distal radial volar locking plate fixation to include previously challenging fracture patterns.
Clinical Applications and Surgical Technique Optimization
Fracture Pattern-Specific Approaches
The versatility of the distal radial volar locking plate system allows for tailored approaches based on specific fracture patterns and patient characteristics. Simple extra-articular fractures benefit from straightforward application techniques that focus on restoring radial length and correcting angulation deformities. The locking mechanism provides reliable maintenance of reduction even in cases where bone quality is compromised, making this an ideal solution for elderly patients with osteoporotic bone stock.
Complex intra-articular fractures require more sophisticated surgical planning and execution, leveraging the advanced features of modern distal radial volar locking plates. Surgeons can utilize variable angle screws to achieve subchondral support for depressed articular fragments while avoiding interference with the distal radio-ulnar joint. The ability to place multiple screws through strategically positioned holes ensures adequate fixation of small fragments that are crucial for joint function and long-term outcomes.
Minimally Invasive Fixation Techniques
The refined design of contemporary distal radial volar locking plates has facilitated the development of minimally invasive fixation techniques that reduce surgical trauma while maintaining fixation quality. Smaller incisions and limited soft tissue dissection are possible due to the predictable anatomical fit of pre-contoured plates, which eliminates the need for extensive exposure required for plate bending. These minimally invasive approaches have been associated with reduced postoperative pain, faster recovery times, and improved cosmetic outcomes.
Percutaneous screw insertion techniques can be employed in selected cases, further minimizing surgical trauma while maintaining the biomechanical advantages of locking plate fixation. The precision manufacturing tolerances of modern distal radial volar locking plates ensure consistent threading and locking mechanisms that function reliably even when inserted through limited exposures. This capability has expanded the use of locking plates to outpatient procedures in appropriate cases, reducing healthcare costs and improving patient satisfaction.
Material Science Innovations and Biocompatibility
Advanced Titanium Alloy Compositions
The material composition of modern distal radial volar locking plates represents the culmination of decades of research in orthopedic biomaterials. Advanced titanium alloys, particularly Ti-6Al-4V, provide an optimal combination of strength, biocompatibility, and corrosion resistance that ensures long-term implant performance. The modulus of elasticity of these alloys more closely matches that of bone compared to stainless steel, reducing stress shielding effects that could compromise bone remodeling and long-term structural integrity.
Surface treatment technologies, including anodization and plasma spraying, enhance the biocompatibility and osseointegration potential of distal radial volar locking plates. These surface modifications promote bone-implant interaction while maintaining the mechanical properties essential for fracture fixation. The corrosion resistance of modern titanium alloys ensures that the implant maintains its structural integrity throughout the patient's lifetime, eliminating concerns about long-term degradation that could compromise fixation or cause adverse tissue reactions.
Precision Manufacturing and Quality Control
State-of-the-art manufacturing processes ensure that each distal radial volar locking plate meets stringent quality standards for dimensional accuracy and mechanical performance. Computer numerical control machining and laser cutting technologies enable the production of plates with precise geometries and consistent surface finishes that optimize their clinical performance. Quality control protocols including non-destructive testing and statistical process control ensure that every implant meets or exceeds industry standards for strength and durability.
The manufacturing precision achieved in modern distal radial volar locking plates extends to the locking mechanism itself, where tight tolerances ensure reliable thread engagement and consistent torque requirements. This precision manufacturing enables surgeons to have confidence in the mechanical properties of the implant, allowing for predictable surgical techniques and reliable outcomes. Advanced packaging and sterilization protocols maintain implant integrity from manufacturing through surgical implantation.
Postoperative Management and Rehabilitation Protocols
Early Mobilization Strategies
The superior stability provided by distal radial volar locking plates enables early mobilization protocols that were not possible with traditional fixation methods. The rigid fixation construct allows patients to begin gentle range-of-motion exercises within days of surgery, preventing stiffness and promoting faster functional recovery. Early mobilization has been shown to reduce the incidence of complex regional pain syndrome and improve long-term functional outcomes in patients treated with locking plate technology.
Structured rehabilitation protocols take advantage of the mechanical stability provided by the distal radial volar locking plate to progressively increase activity levels while protecting the healing fracture. The ability to permit early weight-bearing on the affected extremity in appropriate cases facilitates faster return to activities of daily living and improved patient satisfaction. Physical therapy protocols can be customized based on fracture pattern and patient factors, with the reliable fixation provided by locking plates serving as the foundation for accelerated recovery programs.
Long-term Monitoring and Outcomes Assessment
Long-term follow-up studies of patients treated with distal radial volar locking plates have demonstrated excellent functional outcomes and high rates of fracture union. The stable fixation provided by these implants typically results in anatomical healing with restoration of normal wrist biomechanics. Radiographic monitoring protocols focus on assessing fracture healing progression and identifying any signs of implant-related complications, though the incidence of such issues is significantly lower with modern locking plate designs compared to traditional fixation methods.
Outcome assessment tools including patient-reported outcome measures and objective functional testing demonstrate the superior results achieved with distal radial volar locking plates. The ability to maintain anatomical reduction throughout the healing process translates into better long-term function and reduced risk of post-traumatic arthritis. Studies comparing locking plates to other fixation methods consistently show advantages in terms of functional outcomes, complication rates, and patient satisfaction scores.
Future Developments and Emerging Technologies
Smart Implant Integration
The future of distal radial volar locking plates may incorporate smart sensor technologies that provide real-time monitoring of fracture healing and implant performance. Research into embedded sensors capable of measuring load distribution, temperature, and pH changes could provide valuable data about the healing process and alert clinicians to potential complications before they become clinically apparent. These smart implant technologies could revolutionize postoperative care by enabling personalized rehabilitation protocols based on objective healing parameters.
Wireless communication capabilities could allow smart distal radial volar locking plates to transmit data to external monitoring systems, enabling remote patient monitoring and early intervention when necessary. This technology could be particularly valuable for elderly patients or those with multiple comorbidities who may benefit from enhanced monitoring during the critical healing period. The integration of artificial intelligence algorithms could analyze sensor data to predict healing outcomes and optimize treatment protocols.
Biodegradable Locking Technologies
Research into biodegradable materials for orthopedic implants is exploring the potential for distal radial volar locking plates that gradually dissolve as the fracture heals, eliminating the need for implant removal procedures. Advanced polymer compositions and composite materials are being developed that can provide adequate mechanical strength during the healing phase while safely degrading over time. These biodegradable systems could reduce long-term complications associated with permanent implants and eliminate concerns about implant-related artifacts in future imaging studies.
The development of biodegradable distal radial volar locking plates faces significant challenges in achieving the mechanical properties required for stable fracture fixation while ensuring predictable degradation kinetics. However, advances in material science and manufacturing techniques continue to bring these technologies closer to clinical reality. Successful implementation of biodegradable locking plates could represent the next major advancement in fracture fixation technology.
FAQ
What makes distal radial volar locking plates superior to conventional plates
Distal radial volar locking plates offer several key advantages over conventional plates, primarily through their fixed-angle construct that creates a more stable fixation system. Unlike conventional plates that rely on friction and compression, locking plates secure screws at predetermined angles, eliminating screw toggle and maintaining reduction even in poor bone quality. This technology provides superior resistance to loss of reduction and enables early mobilization, leading to better functional outcomes and reduced complication rates compared to traditional plating systems.
How do variable angle screws improve surgical outcomes
Variable angle screw technology in distal radial volar locking plates allows surgeons to place screws at angles up to 15 degrees from perpendicular, providing greater flexibility in fracture reduction and fixation. This capability enables better capture of small fracture fragments, avoidance of critical anatomical structures like tendons and nerves, and optimization of subchondral support in articular fractures. The increased surgical flexibility translates into improved reduction quality and reduced risk of complications, particularly in complex fracture patterns that would be challenging to address with fixed-angle systems.
What is the expected recovery timeline after distal radial volar locking plate surgery
Recovery after distal radial volar locking plate surgery typically follows a structured timeline beginning with early mobilization within the first week post-surgery. Gentle range-of-motion exercises can usually begin 2-3 days after surgery, with progressive strengthening starting around 6-8 weeks once initial fracture healing is confirmed. Most patients achieve functional use of the wrist within 8-12 weeks, with full recovery and return to high-demand activities typically occurring within 3-6 months depending on fracture complexity and individual healing factors.
Are there any long-term complications associated with distal radial volar locking plates
Long-term complications with modern distal radial volar locking plates are relatively uncommon due to improved design and materials. Potential issues may include flexor tendon irritation if the plate is prominent, though refined low-profile designs have significantly reduced this risk. Hardware removal is rarely necessary unless specifically requested by the patient, as modern titanium alloys are highly biocompatible and corrosion-resistant. Studies show excellent long-term outcomes with low complication rates when proper surgical technique and appropriate patient selection are employed.
Table of Contents
- Biomechanical Advantages of Modern Locking Plate Technology
- Refined Design Features for Enhanced Surgical Outcomes
- Clinical Applications and Surgical Technique Optimization
- Material Science Innovations and Biocompatibility
- Postoperative Management and Rehabilitation Protocols
- Future Developments and Emerging Technologies
-
FAQ
- What makes distal radial volar locking plates superior to conventional plates
- How do variable angle screws improve surgical outcomes
- What is the expected recovery timeline after distal radial volar locking plate surgery
- Are there any long-term complications associated with distal radial volar locking plates